Problems related to nasal tube
Difficulty or inability to irrigate the nasal tube
Possible cause(s)
- Tube blockage (eg, debris from residual formula, reflux of stomach contents, improper preparation of medication)
- Incorrect positioning of the tube (eg, end of the tube pressing against stomach walls)
- Pinched tube
- Damaged tube
What to do?
- Try to find the source of the blockage.
- Check the tube for bends, kinks or jamming.
- If solid particles are visible, gently roll the tube between your fingers to try to loosen them, then gently aspirate with a syringe to try and remove particles
- Change your child’s position.
- Try irrigating the tube again.
- If the problem persists:
- try to unblock the tube by slowly injecting warm water before trying to irrigate again;
- repeat several times.
- If the problem still persists and it is a nasogastric tube and you have been taught to replace it.
- In all other situations, rapidly contact your child’s healthcare team.
Difficulty or inability to aspirate stomach (gastric) contents from the nasal tube
Possible cause(s)
- Blocking of the tube (eg, debris)
- Incorrect positioning of the tube (eg, end of the tube pressed against the stomach walls or away from the accumulation of gastric fluid)
- Collapse of the tube, causing the walls of the tube to stick together during attempt to aspirate
- Empty stomach
What to do?
- Check the tube location as taught by your healthcare team.
- If the problem persists, inject 2 to 3 ml of air through the tube.
- Try again to aspirate gastric secretions.
- If the problem persists, reposition your child on the left side, wait 10 to 15 minutes and then try again to aspirate gastric secretions.
- If the problem still persists and it is a nasogastric tube you have been taught to replace it.
- In all other situations, rapidly contact your child’s healthcare team.
- Until the problem is resolved, do not use the nasogastric tube.
Displacement of the nasal tube
Possible cause(s)
What to do?
- Stop the feeding session, if in progress.
- If your child has a nasogastric tube and you can no longer see the mark on the tube and you have been taught, gently pull the tube until the mark reaches the edge of the nostril.
- If your child has a nasogastric tube and the mark on the tube has moved away from the edge of the nostril and you have been taught, remove the tube and reinsert it.
- Once the tube is correctly positioned:
- In all other situations, leave the tube in place and rapidly contact your child’s healthcare team.
Accidental removal of the nasal tube
Possible cause(s)
What to do?
- If your child has a nasogastric tube and you have been taught:
- inspect the tube for damage;
- if the tube is in good condition, clean it, rinse it well and reinstall it.
- In all other situations, rapidly contact your child’s healthcare team.
Difficulty or inability to insert the nasogastric tube (eg, tube coils in the mouth or comes out through the mouth)
Possible cause(s)
- Agitated child (upset, crying)
- Poor insertion technique
- Nasal obstruction (eg, polyps in the nose)
What to do?
- Remove the tube completely.
- Make sure your child is properly positioned; have a second person help you if necessary.
- Review the method of care (eg, lubricate the tube well before insertion).
- Use a method to distract your child as needed. Make sure your child is calm before trying to insert the tube again.
- If necessary, soak the tube in a container of ice water or put it in the freezer for a few moments to make it more rigid and facilitate insertion into the nostril.
- Encourage your child to swallow or give your baby a pacifier to suck while you insert the tube.
- If the problem persists, contact your child’s healthcare team.
Redness around the nostril in a child with a nasal tube
Possible cause(s)
- Skin irritation
- Nasal discharge
- Friction from poorly secured tube
- Pressure sore caused by the tube
What to do?
- Check if the tube is rubbing against the nostril.
- If necessary, reposition the tube, making sure it is securely attached.
- If your child has a nasogastric tube and you have been taught, remove the tube and insert it into the other nostril.
- If the redness persists, contact your child’s healthcare team.
- In all other situations, rapidly contact your child’s healthcare team.
Breathing difficulties (severe coughing, difficulty breathing, noisy breathing, choking, bluish lips, agitation) during nasogastric tube insertion
Possible cause(s)
- Incorrect insertion of the tube into the airway (trachea) instead of the esophagus
What to do?
- Remove the tube immediately.
- Let your child rest and recover: he or she should be able to breathe better quickly. If this is not the case, call 911 immediately.
- When your child is calmer, review the method of care.
- Encourage your child to swallow or give your baby a pacifier while you try to insert the tube again.
- If the problem persists, rapidly contact your child’s healthcare team.
Discharge through the nasal tube
Possible cause(s)
- Broken nasal tube
- Broken cap
- Forgot to put the cap on the tube
- Worn out cap – less watertight (closes poorly or no longer closes)
What to do?
- Discontinue feeding or irrigating, if in progress.
- Try to find the cause of the discharge.
- Put the cap on the end of the tube between feeding sessions, if not present.
- Put a piece of tape on the cap to securely close it between feeding sessions, if necessary.
- If the nasogastric tube or its cap is broken and you have been taught, change it.
- In all other situations, leave the tube in place and rapidly contact your child’s healthcare team.
Bleeding; blood in the nasal tube
Possible cause(s)
- Injury (eg, traumatic insertion of tube)
- Stomach irritation
- Stomach ulcer
- Infection
What to do?
- Remove the tube.
- Rapidly contact your child’s healthcare team.
Problems related to button or enterostomy long tube
Drainage through or around the button or enterostomy long tube
Possible cause(s)
- Button or tube breakage
- Breakage or obstruction of the anti-reflux valve of the button
- Improperly installed or leaking tube port covers
- Blocking of the button or tube
- Displacement or malposition of the button or tube
- Balloon breakage or deflation
- Presence of granulation tissue
- Skin infection under the button
- Child’s condition (eg, constipation, vomiting, slow digestion, abdominal gas, bloating, chronic cough)
What to do?
- Discontinue feeding or irrigation, if in progress.
- Try to find the cause of the discharge.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), has a gastrostomy balloon button or tube and you have been taught, check to see if the balloon of the button or tube is properly inflated.
- Make sure the tube or button extension set is securely attached to your child and that there is no tension on the tubing.
- Check the location of the gastrostomy tube by gently pulling it outward until the internal retention mechanism holding the tube in place is snug against the stomach wall.
- Irrigate the button or the tube with water.
- Place a few clean, dry compresses on the button or at the tube inlet to absorb the flow; change the compresses regularly depending on the amount of flow.
- Keep the skin around the stoma clean and dry as much as possible.
- Protect the healthy skin around the stoma with a barrier cream or petroleum jelly like Vaseline®.
- If the problem persists, and if your child has a stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), and if it is a gastrostomy balloon button or tube and you have been taught, remove the button or the tube and replace it.
- In all other situations, rapidly contact your child’s healthcare team.
Accidental removal of the button or enterostomy long tube
Possible cause(s)
- Mishandling
- Accident
- Pulled out by child
- Too much tension on the tube (eg, incorrect use of dressings around the stoma)
- Insufficient volume of water in the balloon or balloon bursting
- Button or tube breakage
What to do?
- If the stomach is too full, the contents may come out spontaneously from the stoma, as if your child were vomiting.
- Thoroughly clean and dry the skin around the stoma.
- If your child has had the stoma for less than 6 to 8 weeks (or other length of time as recommended by your healthcare team), rapidly contact your child’s healthcare team.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), has a gastrostomy balloon button or tube and you have been taught:
- check if the button (including its balloon) is in good condition;
- if so, clean it, rinse it well and then put it back in place.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team) and he has another type of button or long tube:
- If you are unable to insert the urinary catheter, try a smaller size catheter.
- If you are still unable to insert a urinary catheter into the stoma, put a compress over the stoma opening and immediately contact your child’s healthcare team. A tube or button must be reinstalled very quickly to prevent the stoma from closing.
Red, crusty, moist, thick, red tissue around the stoma: looks like cauliflower or a turtleneck, soft to the touch, bleeds easily and may leak yellowish/brownish, sticky fluid
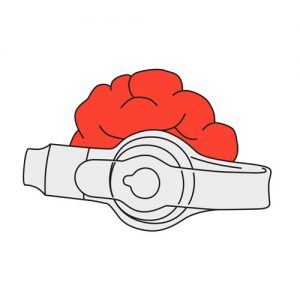
Possible cause(s)
Granulation tissue (or Granuloma or Hypergranulation) which is a reaction of the skin in response to irritation caused by:
- Excessive movement of the button or tube (eg, insufficiently inflated balloon, loose external tube retention disc)
- Incorrect adjustment of the button or tube (eg, button stem too long, tube diameter too small)
- Rubbing of the tube or button inside the stoma
What to do?
- Contact your child’s healthcare team who:
- will evaluate the most appropriate treatment for your child’s condition (eg, medicated cream, silver nitrate),
- will treat the infection, if present,
- will check the appropriateness of changing the button or the tube, if necessary.
While waiting to discuss with your healthcare team:
- If your child has had an the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team) and you have been taught, check that the balloon of the gastrostomy button or tube is not broken and is properly inflated.
- Make sure the tube or button extension set is securely attached to your child and that there is no tension on the tubing.
- Put a few clean compresses around the button or tube if there is any discharge and change the compresses as soon as they get wet.
Redness of the skin around the stoma with or without tenderness, warmth, swelling, discharge different from the usual yellowish or brownish secretions, bad smell and/or fever (≥ 38⁰C rectal or ≥ 37.5⁰C oral or ≥ 37.5⁰C armpit)
Possible cause(s)
- Infection
- Inadequate ostomy care
- Gastric fluid discharge
- Improper fit of the tube or button causing injury to the skin around the stoma
- Incorrect attachment of the tube or extension tube
- Pressure sore
What to do?
- Inspect the button or the tube; check the anti-reflux valve of the button for damage.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team) and you have been taught, check that the balloon of the gastrostomy button or tube is not broken and is properly inflated.
- Make sure the tube or button extension set is securely attached to your child and that there is no tension on the tubing.
- If the problem persists, rapidly contact your healthcare team.
While waiting to discuss with your healthcare team:
- Keep skin clean and dry and leave it exposed to air as much as possible.
- Put a few clean compresses around the button or tube if there is any discharge and change the compresses as soon as they get wet.
Difficulty or inability to aspirate stomach (gastric) contents from the gastrostomy button or long tube
Possible cause(s)
- Empty stomach
- Gastrostomy tube displacement
What to do?
- Change your child’s position and try again to aspirate.
- Make sure the extension set is properly connected.
- Irrigate the button or the long tube with a small amount of water, as recommended by your healthcare team, then retry to aspirate stomach contents.
- If the problem persists, contact your child’s healthcare team.
Difficulty or inability to irrigate the button or the enterostomy long tube
Possible cause(s)
- Blockage of the button, extension set or tube (eg, debris, reflux of stomach contents, improper preparation of medication)
- Pinched tube or extension set
- Button, extension set or long tube damaged (eg, wear)
- Gastrostomy tube displacement
What to do?
- Try to find the source of the blockage.
- Check to see if the button extension set or the tube is bent, kinked or jammed.
- Check if all clamps are open.
- Roll the tube between your fingers if solid particles are visible (to try to remove them).
- Try to aspirate with a syringe if particles are present (to try to mobilize them).
- Disconnect the extension set, if in place, and try to irrigate it to check for blockage; change the extension set if necessary.
- Do not use a sharp object to attempt to unblock the tube or button.
- Do not press too hard on the syringe plunger to attempt to irrigate the button, as excessive pressure may damage the extension set.
- If the problem persists, try to unblock by slowly injecting lukewarm water.
- If the problem persists, if your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), has a gastrostomy balloon button or tube and you have been taught, remove the button or the long tube and change it.
- In all other situations, rapidly contact your child’s healthcare team.
Difficulty or inability to insert gastrostomy balloon button or long tube
Possible cause(s)
- Agitated child
- Poor insertion technique
- Shrinkage of the stoma
What to do?
- Remove the button or the long tube.
- Make sure your child is in the correct position; have a second person help you if necessary.
- Review the method of care.
- Use a method to distract your child if necessary.
- Make sure your child is calm before trying to insert the tube or button again.
- If the problem persists:
- If you are unable to insert a temporary urinary catheter into the stoma, put a compress over the opening and contact your healthcare team immediately. A long tube or button must be reinstalled very quickly to prevent the stoma from closing.
Button or enterostomy long tube breakage (in place)
Possible cause(s)
- Button or tube damaged (eg, wear)
- Manufacturing defect of the button or long tube
- Mishandling
What to do?
- Discontinue feeding or irrigation, if in progress.
- If your child has had the stoma for less than 6 to 8 weeks (or other length of time as recommended by your healthcare team):
- do not change the button or tube;
- contact your healthcare team.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), has a gastrostomy balloon button or tube and you have been taught:
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team) and has another type of button or long tube:
- do not change the button or tube;
- contact your child’s healthcare team.
Disconnection of the extension set during the feeding session
Possible cause(s)
- Accidental disconnection
- Wrong connection of the button extension
What to do?
- Stop the feeding session, if in progress.
- Try to estimate the volume of formula lost.
- Thoroughly clean the button feeding port with soapy water and rinse it well.
- Clean the inside of the extension set port.
- Connect the extension set to the button and irrigate it.
- Resume the feeding session and replace the estimated amount of formula lost during disconnection if possible.
Bleeding through or around the stoma
Possible cause(s)
- Injury
- Irritation
- Granulation tissue
- Infection
What to do?
If the bleeding is severe:
- Discontinue feeding or irrigating session, if in progress.
- Apply pressure with a compress or clean cloth to the site of bleeding.
- Contact your healthcare team immediately.
If the bleeding is light:
- Thoroughly clean and dry the skin around the stoma.
- Keep the skin clean and dry and leave it exposed to air as much as possible.
- Put a few clean compresses around the button or tube and change the compresses as soon as they get wet.
- Contact your child’s healthcare team.
Blood in the (stomach) gastric aspirate from the button or enterostomy long tube
Possible cause(s)
- Injury
- Stomach irritation
- Stomach ulcer
- Infection
What to do?
- Rapidly contact your child’s healthcare team.
Outward movement of the button or enterostomy long tube
Possible cause(s)
- Insufficient volume of water in the balloon or broken balloon
- Excess tension on the tube (eg, use of dressings around the stoma)
- Incorrect adjustment of the tube or button
What to do?
- Stop the feeding session, if in progress.
- Check the tube for excessive tension and reattach it properly, if necessary.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), has a gastrostomy balloon button or tube and you have been taught:
- check the volume of water in the balloon;
- gently push the button stem or tube inward;
- add the necessary amount of water missing from the balloon, if necessary.
- In all other situations, rapidly contact your child’s healthcare team.
Inward movement of the button or enterostomy long tube
Possible cause(s)
- External bolster (to stabilize the tube at skin level) displaced or absent
- Incorrectly secured tube
- Button stem too short
- Incorrect adjustment of the tube or button
What to do?
- Stop the feeding session, if in progress.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), has a gastrostomy balloon button or tube and you have been taught:
- gently pull the tube outward until the internal bolster is seated against the stomach wall;
- make sure the tube’s external bolster is attached to the stomach wall, leaving a space about the thickness of a dime;
- secure the tube to the belly.
- If the problem persists and in all other situations, rapidly contact your child’s healthcare team.
Unable to deflate the balloon of the gastrostomy button or tube (in place)
Possible cause(s)
- Debris in the balloon fill valve
- Button or tube breakage
What to do?
- Make sure that the balloon fill valve is clean and not blocked by debris from formula; clean it if necessary.
- Then firmly insert the syringe into the valve by pushing and turning it a quarter turn; try withdrawing the syringe plunger again.
- If the problem persists and in all other situations, contact your child’s healthcare team.
Inability to rotate the gastrostomy balloon button
Possible cause(s)
- Incorrect button adjustment
- Inadequate ostomy care
What to do?
- Cleanse the skin around the button.
- Then try turning the button again.
- If you are unable to rotate the device, contact your child’s healthcare team.
Problems related to feeding session or general condition of the child
Feeding pump alarms
Possible cause(s)
What to do?
- Press the appropriate button to stop the alarm tone.
- Look at the message on the screen.
- Follow the instructions accordingly.
- If a help screen is available for the alarm, follow the instructions provided.
- If necessary, consult the pump instructions that you have been given.
- If you still cannot resolve the problem, contact your healthcare team.
Difficulty or inability to administer formula or medication through the tube or button (eg, inability to push the plunger on the feeding syringe, blocked or slowed flow of formula by gravity or pump)
Possible cause(s)
- Blockage of the button, extension set, tube or tubing of the bag (eg, inadequate irrigation of the button or tube before use, accumulation of debris, thick texture of the formula, nature of the medication), poor preparation of the medication, interactions between formula and medication, between medications or with gastric secretions, contaminated formula during preparation or poor maintenance of the equipment, which can change the consistency)
- Tube, extension set or tubing clamped
- Button, extension set or tube damaged (eg, worn out)
- Pump malfunction
- Poor administration technique (eg, bag hung too low)
- Intermittent administration of the formula
- Stomach too full
What to do?
- Try to find the source of the blockage.
- Make sure that all tubes are properly connected.
- Check the button extension set, tube or bag tubing for bends, kinks or pinches.
- Make sure clamps are fully open.
- Reposition your child.
- Roll the tube between your fingers if solid particles are visible.
- Try to irrigate the tube or button. Disconnect the extension and irrigate as needed before reconnecting it again.
- Do not use a sharp object to clean the tube or button.
- If necessary, try to unblock by slowly injecting lukewarm water.
- Revise the technique if necessary.
- Look at the message on the screen and if appropriate, follow the instructions accordingly.
- If necessary, consult the pump instructions.
- Change the pump to a back up pump if available, in case of emergency.
- If your child has had the stoma for more than 6 to 8 weeks (or other length of time as recommended by your healthcare team), has a gastrostomy balloon button or tube and you have been taught, change the tube or button.
- In all other situations, rapidly contact your child’s healthcare team.
Nausea and/or vomiting between feeding sessions
Possible cause(s)
- Interval between feeding sessions too short
- Formula administration speed too fast
- Too much formula administered
- Intolerance or allergy to the formula
- Constipation
- Gastric reflux (stomach contents rise up into the esophagus)
- Dumping syndrome (or rapid gastric emptying): the stomach empties too quickly into the intestine
What to do?
- If your child is nauseated, place the child in an upright seated position
- If your child is vomiting, put your child’s head to the side.
In both cases:
- Postpone the next feeding session for 30 to 60 minutes.
- Reduce the amount or rate of formula to be administered, as recommended by your healthcare team.
- If the problem persists, contact your child’s healthcare team.
Nausea and/or vomiting during feeding session
Possible cause(s)
- Formula administration speed too fast
- Excess air in the stomach
- Too much formula administered
- Formula too cold
- Formula too concentrated
- Intolerance or allergy to the formula
- Contamination of the formula (during preparation, poor maintenance of the equipment)
- Gastric reflux (stomach contents rise up into the esophagus)
- Gastric emptying is fast or too slow (the stomach empties too quickly or too slowly into the intestine)
- Change in administration schedule
- Constipation
- Infection
What to do?
If your child has nausea:
- Place the child in an upright seated position, if possible.
- Slow down or stop feeding until your child is comfortable and then resume feeding.
- If the problem persists, contact your child’s healthcare team.
If your child vomits:
- Turn your child’s head to the side.
- Stop feeding for 30 to 60 minutes and then start again more slowly.
- If the problem persists, contact your child’s healthcare team.
Breathing difficulties (eg, coughing, choking, noisy and/or wheezy breathing, increased work of breathing (retraction of the skin around the ribs and collarbones), bluish discoloration of the lips and skin) during a feeding session
Possible cause(s)
- Aspiration (accidental entry of formula into the lungs): caused by improper positioning of the child or the nasal tube, vomiting or gastric reflux
- Condition of the child
- Respiratory infection
What to do?
- Stop the feeding session immediately.
- Stay calm and reassure your child.
If your child is in respiratory distress:
- Call immediately 911.
- Begin CPR as taught.
If your child is not in respiratory distress:
- Put your child in a sitting position or turn the child onto the side to make breathing easier.
- If your child has a nasogastric tube, check the tube location. If it is not in the stomach, remove it immediately and reinsert it when your child becomes calm again.
- If your child has a button or another type of tube, rapidly contact your child’s healthcare team.
- If your child has other discomforts in addition to breathing difficulties, rapidly contact your child’s healthcare team.
Bloating / swelling of the belly during feeding session
Possible cause(s)
- Formula administration speed too fast
- Excessive swallowing of air (eg, in children with non-invasive ventilatory support, crying)
- Excess gas produced by digestion or infection
- Too much formula at each feeding session
- Intolerance to the formula
- Poor absorption of the formula
- Gastric emptying too slow (the stomach contents empty too slowly into the intestine)
- Bowel obstruction
- Condition of the child
What to do?
- If your child has severe abdominal pain and/or other discomforts (eg, vomiting), stop the feeding session and immediately contact your child’s healthcare team.
- If this is not the case, reduce the flow rate of the formula, according to your child’s tolerance.
- If the problem persists:
- stop the feeding session for 30 to 60 minutes;
- if you have been instructed, decompress (or vent) the button or tube to let air out of the stomach.
- If your child does not have any more discomfort afterwards, resume the feeding session by increasing the speed of flow progressively.
- If the problem persists, contact your child’s healthcare team.
Bloating / swelling of the belly between feeding sessions
Possible cause(s)
- Excessive swallowing of air (eg, in children with non-invasive ventilatory support, crying)
- Excess gas produced by digestion or infection
- Too much formula at each feeding session
- Intolerance to the formula
- Poor absorption of the formula
- Gastric emptying too slow (the stomach contents empty too slowly into the intestine)
- Bowel obstruction
- Condition of the child
What to do?
- If your child has severe abdominal pain and/or other discomforts (eg, vomiting), stop the feeding session and and immediately contact your child’s healthcare team.
- If this is not the case and if you have been instructed, decompress (or vent) the button or tube to let air out of the stomach.
- Be sure to close the tube cap tightly between feeding sessions.
- If your child can also feed by mouth, eliminate liquids and foods that cause gas or intolerance, as recommended by your healthcare team.
- If the problem persists, contact your child’s healthcare team.
Abdominal pain during feeding session
Possible cause(s)
- Formula administration speed too fast
- Too much formula at each feeding session
- Formula too cold
- Excess air in the stomach
- Gastric emptying too slow (the stomach contents empty too slowly into the intestine)
- Intolerance to the formula
- Constipation
- Gastrointestinal problems (eg, intestinal obstruction)
- Infection
What to do?
- If your child has severe abdominal pain, stop the feeding session and and immediately contact your child’s healthcare team.
- If the pain is fairly mild, reduce the flow rate of the formula, according to your child’s tolerance
- If the problem persists, discontinue administration for 30 to 60 minutes, which may help reduce symptoms and then gradually resume the feeding session.
- If the problem still persists and you have been taught, decompress (or vent) the button or tube to let air out of the stomach and then gradually resume the feeding session.
- If the problem persists, contact your child’s healthcare team.
Diarrhea (soft or liquid stools more frequent than usual) with or without cramps and/or abdominal pain
Possible cause(s)
- Infection
- Formula administration speed too fast
- Use of formulas that have passed the expiry date
- Contamination of the formula (during preparation, poor maintenance of the equipment)
- Side effects of medication (eg, antibiotics)
- Intolerance to the formula
- Movement of the tube or button
- Too much fiber in the diet
- Food allergies or intolerances
- Dumping syndrome (or rapid gastric emptying): the stomach contents empty too quickly into the intestine.
- Condition of the child
What to do?
- Discontinue feeding session if in progress.
- If your child has bloody diarrhea, fever or episodes of diarrhea are frequent, immediately contact your child’s healthcare team.
- If this is not the case, check your child’s hydration level (thirst, dry lips and tongue, darker urine, with a strong odour and in small quantities, weakness, dizziness).
- If your child seems dehydrated or is having many more stools than usual, immediately contact your child’s healthcare team.
- If your child is adequately hydrated, delay feeding for 30 to 60 minutes to relieve symptoms; resume feeding session more slowly over the next few hours.
- Review the cleanliness guidelines for formula preparation and storage recommendations (including in the hanging bag).
- Check the expiry date of the formula: discard products that are past their expiry date or return them to the pharmacy.
- If the problem persists, consult your child’s healthcare team.
Constipation (infrequent and/or difficult to pass stool for more than a day) with or without nausea, vomiting, abdominal bloating, cramps and/or abdominal pain
Possible cause(s)
- Insufficient hydration
- Inactivity
- Lack of fibre in the diet
- Change of formula
- Side effects of medication
- Intolerance to the formula
- Change of medication
- Condition of the child
What to do?
- Make sure your child gets all the fluid he or she needs.
- Increase the amount of physical activity your child gets, if possible.
- Contact your healthcare team for advice on nutrition (eg, increasing dietary fibre).
- If the problem still persists, contact your child’s healthcare team.
Dry mouth
Possible cause(s)
- Insufficient hydration
- Lack of mouth stimulation
- Side effects of medication
- Condition of the child
What to do?
Yellowish or greenish vomiting (bile) or yellowish or greenish liquid visible in the feeding tube
Possible cause(s)
- Movement of the gastrostomy tube or urinary Foley™ catheter into the intestine
- Bowel obstruction
- Intussusception or intestinal invagination (folding of the intestines on top of each other, like a telescope: most common with nasojejunal or gastrojejunal tubes)
What to do?
- Discontinue feeding session or irrigation, if in progress.
- Check that the gastrostomy tube or urinary Foley™ catheter is in the right place, as taught to you by your healthcare team.
- If not, reinstall the tube or catheter correctly.
- If the tube or catheter is in the right place and the problem persists, immediately contact your child’s healthcare team.
One or more of these symptoms between feeding sessions: Headaches; Chest pain; Vomiting; Blurred vision; Perspiration (sweating); Pallor (pale skin); Fatigue or irritability; Tremors (shakiness); Convulsions
Possible cause(s)
- Hypoglycemia (low blood sugar)
- Infection
- Dumping syndrome (or rapid gastric emptying): the stomach contents empty too quickly into the intestine
What to do?
- If your child is having a convulsion or is not responsive, immediately contact 911.
- If not, check your child’s blood glucose, if already discussed and you have been taught by your healthcare team.
- Rapidly give your child an additional source of sugar as recommended by your healthcare team in this situation.
- Immediately contact your child’s healthcare team.
One or more of these symptoms during and/or after feeding session: Headaches; Chest pain; Strong thirst; Weakness; Agitation; Irritability; Abdominal cramps; Diarrhea; Urine more often than usual
Possible cause(s)
- Hyperglycemia (high blood sugar)
- Infection
- Dumping syndrome (or rapid gastric emptying): the stomach contents empty too quickly into the intestine
What to do?
- Check your child’s blood glucose, if already discussed and you have been taught by your healthcare team.
- Immediately contact your child’s healthcare team.
One or more of these symptoms: Increased thirst; Dry and sticky tongue; Dry and chapped lips; Hollow or sunken eyes; Darker urine, strong odor and in smaller quantities than usual; Urine less often than usual; Weakness; Dizziness
Possible cause(s)
- Dehydration because of low water intake or significant fluid loss (eg, through vomiting, diarrhea, excessive sweating, fever, certain medications)
What to do?
- Rapidly contact your child’s healthcare team.
- Give your child rehydration formulas (eg, Pedialyte™, Gastrolyte™), if recommended by your healthcare team.
One or more of these symptoms: Faster breathing, difficulty breathing; Swelling especially in the legs, feet and around the eyes; Quick and sudden weight gain
Possible cause(s)
- Fluid overload in the body
- Low protein levels in your child
- Infection
- Condition of the child
What to do?
- Immediately contact your child’s healthcare team.









