Indications:
- Aspiration of nasopharyngeal secretions (through the nose to the pharynx) is necessary when your child is not able to independently clear secretions that accumulate in the back of the throat.
- Below is a suggested method that can serve as a guide; discuss the specific type of medical supplies and equipment used for your child with the healthcare team.
Considerations:
- Excessive aspiration can irritate the fragile lining of the mouth and pharynx, increase the production of secretions and/or predispose your child to respiratory infections. Limit aspiration to an as needed basis.
- The pressure regulator of the suction device should be adjusted based upon the recommendations of the healthcare team; in general, the level of pressure recommended varies according to the age of the child:
- Newborns (one month and less): between 60 and 80 mmHg
- Infants: between 80 and 100 mmHg
- Children: between 100 and 120 mmHg
- Adolescents: between 100 and 150 mmHg.
- If the secretions are very thick, a higher pressure may be required. To prevent tissue injury, gradually increase the pressure and watch carefully for signs of bleeding or discomfort. Discuss this with your healthcare team.
- If your child has a tracheal cannula with a balloon, then nasopharyngeal aspiration is recommended prior to deflating the balloon in order to prevent secretions from moving from the throat into the lungs.
- Nasopharyngeal aspiration is done with a flexible suction catheter.
- Never use:
- The same catheter to aspirate nasopharyngeal and tracheobronchial secretions; instead use a separate catheter in each location to minimize transfer of bacteria from the mouth into the lungs.
- The flexible catheter used to aspirate oral secretions to also aspirate nasopharyngeal secretions, unless the catheter has been well cleaned beforehand.
- Children often cough during this procedure, especially when the suction catheter is placed in the mouth.
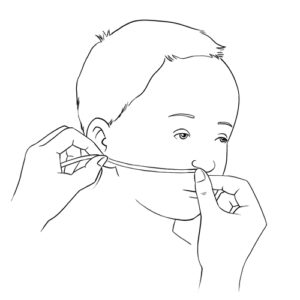
- Catheter insertion length: To avoid inserting the suction catheter too deeply into the trachea, it is important to establish a maximal insertion length; refer to your healthcare team or use the guideline provided here:
- take a previously used catheter or a new catheter that remains in its envelope;
- place the end of the catheter at the tip of your child’s nose and measure the distance to the lobe of your child’s ear on the same side;
- note the number on the catheter that corresponds to this distance (reference point);
- to avoid damaging your child’s trachea, do not insert the catheter further than this predetermined distance.If you are unable to aspirate secretions using this length of catheter insertion, recheck your measurements. As your child grows, the maximal catheter insertion length will change; check with your healthcare team to determine how often this length should be reassessed.
- If your child is unable to clear nasal secretions effectively, then it is important to clean the nose well before and after nasopharyngeal aspiration in order to minimize the risk of respiratory infections. If your child can clear nasal secretions (for example, by blowing the nose) then aspiration of nasal secretions may not be required.
- Refer to your healthcare team to determine which method of nasal hygiene is recommended, how often it should be completed and which type of rinsing solution should be used.
- Determine if you require a second person to help hold your child in a secure position (for example, if your child is young or moving around a lot).
- Good handwashing is essential before and after providing care.
- Ensure the comfort of your child during care by using different positioning and distraction techniques.
Frequency:
- The frequency of nasopharyngeal aspiration depends upon the quantity of retained secretions. Check with your healthcare team to determine the recommended frequency for your child.
- Wait at least 30 minutes after meals before aspirating secretions, to reduce the risk of vomiting.
- Allow at least a 30 minute break between aspirations, if possible.
Required materials:
The methods of care below are illustrated with a LSU suction device.
Refer to your child’s healthcare team if the material or the sequence of steps you have been taught is different than those described.








